Imagine waking up and realizing your body no longer follows your commands. For thousands of people every year, a car accident, a bad fall, or an act of violence turns this nightmare into a reality. Spinal Cord Injury is damage to the spinal cord that causes a temporary or permanent loss of motor, sensory, and autonomic function below the point of injury. Commonly known as SCI, it isn't just about paralysis; it's a complete rewrite of how a person interacts with the world. While the initial shock is overwhelming, the goal of modern medicine isn't just survival-it's about reclaiming as much independence as possible through aggressive rehab and smart technology.
What Actually Happens During Function Loss?
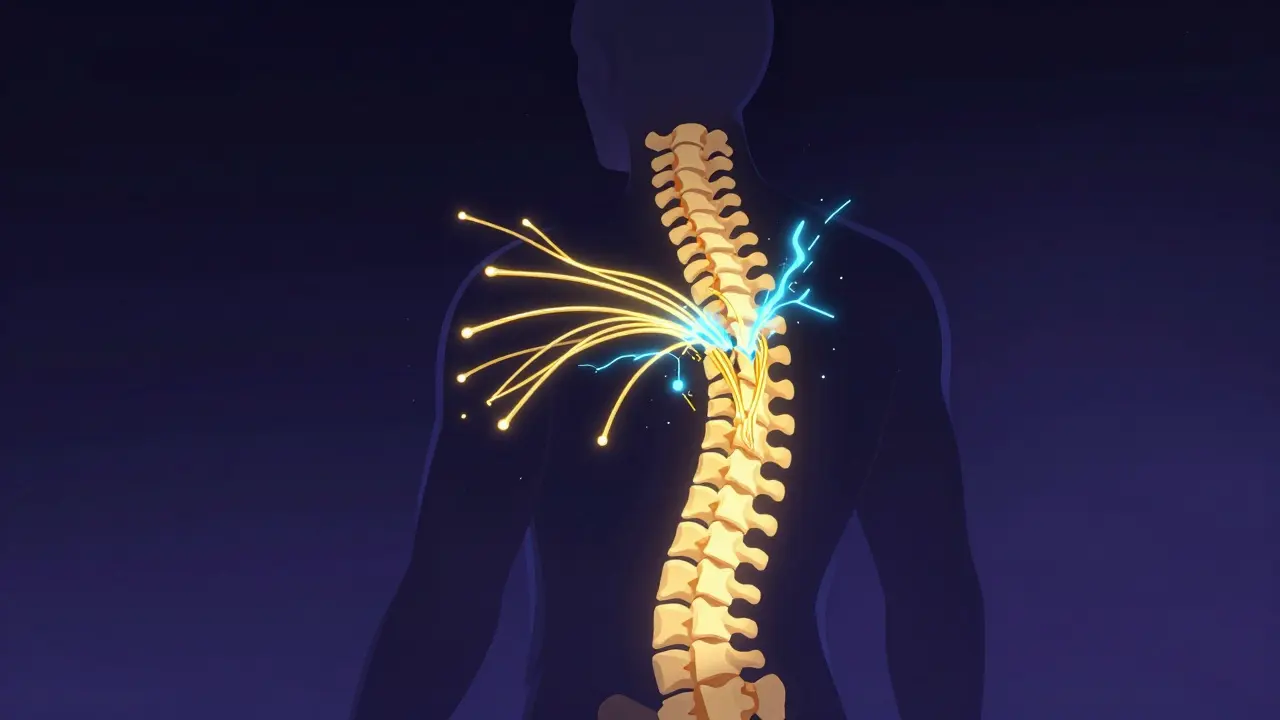
When the spinal cord is damaged, the "communication lines" between the brain and the rest of the body are cut or frayed. This leads to a loss of control over muscles (motor function), the inability to feel touch or pain (sensory function), and a breakdown in automatic body processes like blood pressure and bladder control (autonomic function). The impact depends entirely on where the injury happened and how severe it is.
If the injury is "complete," the spinal cord is fully severed or crushed, meaning no signals get through. If it's "incomplete," some pathways remain intact. This distinction is huge for recovery. For instance, about 59% of people with incomplete paraplegia eventually regain the ability to walk, whereas only 1-3% of those with complete injuries do. It's a stark reminder that every single nerve fiber saved counts.
The level of the injury also dictates the challenges. A high cervical injury (C1-C4) might mean someone needs a ventilator to breathe, while a thoracic injury might leave the arms fully functional but the legs paralyzed. This is why a "one size fits all" approach to recovery simply doesn't work.
The Roadmap to Recovery: Rehab Stages
Rehab doesn't start months later; it starts the moment the patient is medically stable, often within 24 to 72 hours. The process is a marathon divided into three critical phases.
The Acute and Subacute Phase
The first 6 to 12 weeks are all about survival and prevention. When muscles go flaccid (limp), they can shorten, leading to permanent joint stiffness called contractures. To stop this, therapists perform passive range of motion (ROM) exercises. If a patient has spasticity (muscle stiffness), these exercises might happen three times a day. This phase also focuses on respiratory care-things like assisted coughing and incentive spirometry-which can cut pneumonia rates by 65% for those with high cervical injuries.
The Intensive Inpatient Phase
This is the "heavy lifting" part of recovery. Patients typically undergo at least three hours of therapy five days a week. It's a team effort involving neuropsychologists, physical therapists, and occupational therapists. The focus shifts to active-assisted exercises and learning how to move from a bed to a wheelchair safely. This is where the most significant functional gains happen; many people with incomplete injuries reach 80-90% of their potential recovery within the first year.
Community Reintegration
Around the 3-to-6-month mark, the focus moves toward the real world. Outpatient sessions help patients navigate their homes, return to work, or get back into social circles. A huge part of this is psychological. Peer counseling is often the "secret sauce" here, with over 80% of patients reporting that talking to others who have "been there" significantly helps them adjust to their new life.

Cutting-Edge Assistive Devices and Tech
Technology is rapidly bridging the gap between what the body can't do and what the person wants to achieve. We've moved far beyond just basic wheelchairs.
Functional Electrical Stimulation (or FES) is a game-changer. By using electrical pulses to trigger muscle contractions, FES cycling helps maintain leg muscle mass and improves cardiovascular health. In fact, FES cycling can increase peak oxygen consumption by 14.3%, far outperforming standard arm cycling.
Then there are the "robots." Powered lower-limb exoskeletons, like those from Ekso or ReWalk , allow people with paralysis to stand and take steps. While these are amazing for morale and bone density, they aren't perfect. They're expensive and energy-draining, often limiting a session to just 30-45 minutes. For those with severe breathing issues, the FDA-approved implantable diaphragm pacing systems have reduced ventilator dependence by 74% for some patients.
| Technology | Primary Benefit | Main Trade-off | Target Injury Level |
|---|---|---|---|
| FES Cycling | Muscle maintenance & heart health | High out-of-pocket cost | Paraplegia / T-levels |
| Exoskeletons | Upright mobility & bone density | Short session limits (30-45 min) | Complete/Incomplete Paraplegia |
| Diaphragm Pacing | Reduced ventilator use | Requires invasive surgery | High Cervical (C3-C5) |
| TPAD (Tethered Pelvic Assist) | Enhanced balance training | Available mostly in research labs | Incomplete SCI |

The Hard Parts: Managing the "Invisible" Challenges
Recovery isn't just about walking or moving arms; it's about the things people don't talk about at dinner parties. Neurogenic bowel and bladder management is a daily reality that can take up to 90 minutes of a person's day. Without a strict routine, these issues can lead to kidney failure or severe infections.
Spasticity-the involuntary tightening of muscles-affects roughly 65-78% of people with SCI. Managing it usually requires a cocktail of oral medications like baclofen and targeted botulinum toxin injections. When done right, this combination can reduce spasticity scores by 40-60% for most patients.
Then there's the financial burden. While insurance helps, it rarely covers everything. Specialized seating for wheelchairs can leave families with out-of-pocket costs between $1,200 and $3,500. This financial stress, combined with the mental toll of the injury, is why the psychological aspect of rehab is just as important as the physical one.
Pro Tips for Caregivers and Families
If you're supporting someone with an SCI, your own health is at risk if you don't use the right techniques. About 32% of secondary shoulder injuries in caregivers are caused by improper transfer techniques (moving the patient from bed to chair). Always use a gait belt and keep your back straight.
Consistency is the biggest hurdle. A survey by the United Spinal Association found that 68% of patients stop their home exercise programs within six months. The key to beating this is accountability. Set a schedule, use a tracking app, or join a support group to keep the motivation high long after the official rehab center has discharged the patient.
Can a complete spinal cord injury ever be reversed?
Currently, medical science cannot "cure" a completely severed spinal cord. However, functional recovery is possible. While only 1-3% of complete paraplegics regain ambulatory function, many can regain significant independence using assistive technology and adaptive strategies. Emerging research into brain-computer interfaces is showing promise in restoring some hand function for cervical injuries.
How soon should rehabilitation begin after an injury?
Rehabilitation should ideally begin within 24 to 72 hours after the patient is medically stabilized. Early intervention is critical to prevent secondary complications like muscle atrophy, joint contractures, and respiratory infections, and it maximizes the window for neurological recovery.
What is the difference between paraplegia and quadriplegia?
Paraplegia typically refers to paralysis of the lower half of the body, including the legs, usually resulting from injuries in the thoracic or lumbar sections of the spinal cord. Quadriplegia (or tetraplegia) involves paralysis of all four limbs and the torso, usually resulting from injuries in the cervical (neck) section of the spinal cord.
Are robotic exoskeletons a replacement for wheelchairs?
No, not currently. Exoskeletons are primarily used as therapeutic tools to improve bone density, reduce spasticity, and provide psychological benefits. They are too slow and energy-intensive for daily travel, and most sessions are limited to 30-45 minutes. Wheelchairs remains the primary mode of independent mobility.
How do I manage spasticity at home?
Management should always be guided by a doctor, but it typically involves a mix of daily stretching, passive range of motion exercises, and medications like baclofen. For more stubborn muscle groups, botulinum toxin injections may be used to relax the muscles and reduce pain.



Ryan Hogg
April 11, 2026 AT 20:53Reading this just reminds me of how fragile everything is. I spent three years in a dark place after my own accident and the trauma just never really leaves you. It's like you're a ghost in your own life and no one understands the actual void you feel every single morning when you wake up. The physical rehab is one thing, but the soul just stays broken. I don't know how some people just 'adjust' because for me it's just a constant cycle of grief and remembering what I lost. It's just exhausting to even think about the future.
danny Gaming
April 12, 2026 AT 08:01wow typical US medical hype stuff lol these robots are way overpriced junk and probably made in china anyway why act like it's some miracle when the cost is insane smh
Chad Miller
April 14, 2026 AT 03:28some ppl r really just lazy and dont do the exercises theyre told’ too bad the healthcare systm is such a joke here
emmanuel okafor
April 15, 2026 AT 05:23it is interesting how the mind finds a way to live even when the body is still. we are all just trying to find peace in a world that is often too loud
Julie Bella
April 16, 2026 AT 16:53I totaly agree that the acountability part is the most importnt!! I lawayz tell my friends that if you dont have a schedule you're just failing yourself!! 💖 You gotta stay strong and not let the laziness win!!
Rakesh Tiwari
April 17, 2026 AT 14:24Oh, absolutely. Because clearly, spending thousands on a chair that barely works is the pinnacle of modern medical success. Truly inspiring stuff.
Camille Sebello
April 17, 2026 AT 17:50The bowel management part is so vital... People ignore it!! It's disgusting but necessary!!!
Simon Jenkins
April 18, 2026 AT 01:17The sheer audacity of presenting these 'robotic' gadgets as a revolution is simply laughable. Let us be perfectly clear: an exoskeleton that lasts forty minutes is not a tool; it is a toy for the wealthy to feel a fleeting sense of normalcy. It is a tragic farce of a solution that treats the symptom while the patient remains a prisoner to a bankrupt insurance system. The drama of 'reclaiming independence' is nothing more than a marketing script written by corporations who profit off of desperation. It is utterly pedestrian to think this is the ceiling of recovery. I find it absolutely grating that we pretend this is progress when it's barely a step forward in a thousand-year slog of medical mediocrity. Give me a real breakthrough or give me silence, because this halfway-house of technology is simply an insult to the actual struggle of the injured. It's a theatrical performance of hope without any actual substance behind the curtain. I am practically aghast at how easily people swallow this narrative.
Sarina Montano
April 19, 2026 AT 10:46FES cycling is actually a kaleidoscope of possibilities for cardiovascular health! It's such a vibrant way to keep the heart pumping when the usual paths are blocked. I've seen it breathe life back into muscle groups that seemed totally dormant, which is just magical in a clinical sense.